
Hope for Healing Brain Damage from Getting Shot, Dementia, Etc!
Twenty years ago, medicine did not believe that neurological damage could be reversed. If one were to incur brain damage, whether from a traumatic injury like being shot, drug use, dementia, poisoning, etc, it was considered a done deal. This is because of the prior belief that adult brains cease to grow new neurons, being stuck with a finite number from which losses can be deducted but no gains added. However, newer research has uncovered hope for those that have sustained brain damage. Scientific evidence now exists that the human brain actually generates new brain cells in a process known as neurogenesis well into adulthood, with even people in their nineties producing new brain cells! While it is true that the production rate does decrease with age, there are certain therapies that can accelerate neurogenesis, which is especially applicable in instances of trauma.
Below, I will explore three different techniques that have produced positive effects on injured brains, as confirmed by medical testing.
Nutrition, Sleep, Supplements, & Exercise

This first technique is one you can actually replicate yourself at home. Pretty much all it involves is taking really good care of yourself!
A research team wishing to study a set of interventions for improving brain damage needed study subjects with signs of brain injury. These they found at an outpatient neuropsychiatric clinic, where they selected thirty retired professional football players for their study. Football players are an especially good population to look at because of the prevalence of head trauma in their occupation.
Initial data was collected from the subjects using SPECT (Single Photon Emission Computed Tomography) imaging to get a snapshot of cerebral blood flow and a neuropsychological test to measure cognitive functioning.
With these starting measurements collected, the subjects were then educated to follow a set of healthy interventions. They were to take just under a tsp and a half of fish oil a day, a potent multi-vitamin, a supplement containing ginkgo and vinpocetine to increase cerebral blood flow, acetyl-l-carnitine and huperzine A to boost acetylcholine levels in the brain, and (finally) alpha-lipoic acid and n-acetyl-cysteine as antioxidants. The subjects were educated on getting good nutrition, adequate sleep, addressing sleep apnea, and exercising regularly. Overweight subjects were encouraged to lose weight. Recreational drugs, including cigarettes, were completely cut out, though alcohol was allowed in smaller quantities.
The trial lengths varied widely by participant, lasting as short as two months or as long as one year, and the average was approximately six months. Upon completion, the former football players again underwent a SPECT scan and retook the neuropsychological test. The results? Blood flow had visibly increased in multiple brain regions, such as the prefrontal cortex (known as the executive functioning area of the brain), the occipital lobes (vision region), and cerebellum (responsible for voluntary movements and balance). The neuropsychological test confirmed a marked improvement on average in the subjects’ ability to remember things, process information, concentrate, and reason. Not a bad payoff for persisting at good habits for just six months!
Hyperbaric Oxygen Therapy

Unlike the above scenario, hyperbaric oxygen therapy (or HBOT) is not something you can do at home. This medical treatment involves breathing pure oxygen for one to two hours while either sitting or lying in a specialized tank or chamber that has been pressurized up to three times above standard atmospheric pressure. The pressure forces the oxygen deep into tissues, where it reduces inflammation, combats infection, and stimulates the formation of blood vessels, thereby promoting healing. HBOT is not a new healing modality; starting in the 1930s, it was used for treating decompression sickness. A rough prototype of a hyperbaric chamber can be traced as far back as the mid-1600s!
Though HBOT has been around for some time, research into its benefits is ongoing. During one such study, a team of researchers decided to look into the pros and cons of HBOT for treating PTSD and persistent post-concussion syndrome in military veterans. Military veterans are an excellent population for researching brain damage, because of the prevalence of injuries like being shot, exposed to explosives, and so forth. Twenty-nine military veterans, all of which had experienced brain trauma and some of which had PTSD, underwent psychological and neuropsychological tests, SPECT scans of their brains, and physical exams. These tests, scans, and exams were administered a second time after one HBOT session and then a third (and last time) after thirty-nine HBOT sessions that took place over a period of about a month.
The pros of HBOT were impressive. The veterans experienced significant improvements in their memory, anxiety and depressive issues, cerebral blood flow, PTSD symptoms, hand dexterity, and even IQ! Positive changes were seen after just one session. Upon completion of the treatments, the veterans reported a higher quality of life and a decreased reliance on psychiatric drugs. Most experienced either a decrease or a complete stop of suicidal thoughts and panic attacks. Though the initial brain scans revealed regions of damage in the subjects’ brains, three-quarters of these regions became virtually indistinguishable post-treatment compared to those of healthy brains. When interviewed six months after the treatment ended, most of the veterans continued to see improvements.
Regarding the cons associated with HBOT, a minority of the subjects experienced side effects – barotrauma to the ear and bronchospasm (both reversible), anxiety, and a short-term worsening of symptoms. Barotrauma is unfortunately a known side effect of HBOT that might not make it a good fit for people whose ears can not handle pressure differences. If you suffer from ear pain when flying, undergoing HBOT is probably not a good idea.
Deep Brain Stimulation
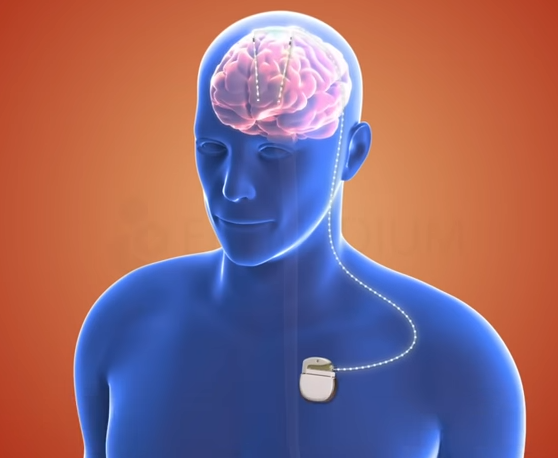
For those who are not afraid of invasive treatments, getting a brain implant is a third option for helping with brain injury. In deep brain stimulation, electrodes are surgically placed in the brain region specific to a problem area. These electrodes are connected via a wire running under the skin to a neurostimulator device implanted in the patient’s chest. This device behaves like a pacemaker, sending electrical pulses up the wire to the electrodes to stimulate the brain.
Examples exist of people with brain injuries who have benefited from deep brain stimulation. Almost two decades ago, Gina Arata got into a car accident and sustained a TBI (traumatic brain injury). It left her with an inability to concentrate or read, a propensity to speed and get into car accidents, and also memory loss, a quick temper, and a droopy foot. Seventeen years later, she elected to receive an experimental deep brain stimulation device. The changes were immediate – Gina’s memory became functional, she no longer trips, her speeding issues and temper resolved, and her ability to read was restored.
Research trials with other participants revealed this incredible restoration of functioning with the deep brain stimulation device. Those that couldn’t read or do homework were able to do so again. They could play video games or watch TV once more. Sleepiness issues were lessened. However, when the devices were switched off, it seems that the improvements petered away.
While deep brain stimulation is not intended to fix or regenerate the brain itself but rather operate as more of a crutch, evidence exists that it can promote neurogenesis. For over twenty years at this point, deep brain stimulation devices have been available on the market to treat Parkinson’s. In postmortems of Parkinson’s patients who had used this device and later passed away for other reasons, scientists have detected increased levels of cell growth compared to untreated brains.
So, there you have it – three different methods to induce neurogenesis, listed from least to most invasive.
References:
1. Tobin, M.K., Musaraca, K., Disouky, A., et al. (2019, June 6). Human Hippocampal Neurogenesis Persists in Aged Adults and Alzheimer’s Disease Patients. Cell Stem Cell, Vol. 24 (6). https://pubmed.ncbi.nlm.nih.gov/31130513/
2. Amen, D.G., Wu, J.C., Taylor, D., & Willeumier, K. (2011, April 8). Reversing Brain Damage in Former NFL Players: Implications for Traumatic Brain Injury and Substance Abuse Rehabilitation. Journal of Psychoactive Drugs, Volume 43 (1). https://www.tandfonline.com/doi/full/10.1080/02791072.2011.566489#abstract
3. Smolle, C., Lindenmann, J., Kamolz, L., & Smolle-Juettner, F.M. (2021, Jan. 8). The History and Development of Hyperbaric Oxygenation (HBO) in Thermal Burn Injury. Medicina (Kaunas), Vol. 57 (1). https://pmc.ncbi.nlm.nih.gov/articles/PMC7827759/
4. Harch, P.G., Andrews, S.R., Fogarty, E.F., et al. (2017, Oct. 17). Case control study: hyperbaric oxygen treatment of mild traumatic brain injury persistent post-concussion syndrome and post-traumatic stress disorder. Medical Gas Research, Vol. 7 (3). https://pmc.ncbi.nlm.nih.gov/articles/PMC5674654/
5. Deep brain stimulation. (2026, Mar. 17). Mayo Clinic. https://www.mayoclinic.org/tests-procedures/deep-brain-stimulation/about/pac-20384562#:~:text=A%20pacemakerlike%20device%20controls%20the,number%20of%20conditions%2C%20such%20as:
6. Bai, N. & Erickson, M. (2023, Dec. 4). Brain implants revive cognitive abilities long after traumatic brain injury. Stanford Medicine. https://med.stanford.edu/news/all-news/2023/12/traumatic-brain-injury-implant.html
7. Vedam-Mai, V., Gardner, B., Okun, M.S, et al. (2014, Mar. 3). Increased Precursor Cell Proliferation after Deep Brain Stimulation for Parkinson’s Disease: A Human Study. PLOS One, Vol. 9 (3). https://pmc.ncbi.nlm.nih.gov/articles/PMC3940428/#:~:text=Close%20to%20the%20lead%20placement,placement%20in%20PD%2DDBS%20brains.
Other Articles: